In her monthly leadership series, Dr. Barbara Schmidtman—vice president of cancer health operations at Corewell Health West—offers her perspective on addressing workforce-related issues through effective leadership practices. Find all her posts in this blog series on the ACCC website.
Last month, I had the privilege of representing the ACCC Oncology Workforce Subcommittee at the 39th National Oncology Conference—hosted in West Palm Beach, Fla., from Oct. 12 to 14—and speak about findings from the association’s 2022 Mini Z burnout survey, which was also conducted in 2019.
For those of you who are unfamiliar with the Mini Z burnout survey, it is a statistically validated tool that measures burnout in healthcare professionals. Originally the tool was utilized to measure burnout among physicians, but, as time has progressed and the implications of burnout have been further explored, it has also been validated for use with other healthcare professionals, including advanced practice providers (APPs). The survey asks a series of questions that focus on outcomes and drivers of burnout, such as job satisfaction, stress, workplace atmosphere, workload, electronic health record (EHR) proficiency, and time spent in the EHR at home, including a qualitative question to understand how each individual defines burnout via a series of five pre-constructed answers—determining the extent to which an individual is burned out or not.
We know that burnout in the oncology profession is real, considering a lot of literature on healthcare burnout existed prior to the COVID-19 pandemic due to the complex nature of our work. We must deliver difficult news to patients and their families, provide complex treatments, deal with various payer rules that seem to continuously change, and, ultimately, deal with death—sometimes we watch patients, who we have grown to love, pass away. In conducting the Mini Z survey in 2022, ACCC’s intention was to measure levels of stress and burnout across all the oncology professionals that make up the multidisciplinary cancer care team for the first time, as well as to compare results from these professionals between 2019 and now.
Comparing Results: 2019 to Now
There were some limitations that I’d like to note when looking at the Mini Z results comparison from 2019 to 2022. The first was the number of participants; this number drastically dropped in 2022. There were 327 participants in 2019, whereas, in 2022, only 118 people participated in the survey. This alone could speak to a potential indication of healthcare burnout—less people felt compelled to participate in the survey or were simply too burned out to open the email. The other notable limitation is that there could be a variation in who answered the survey in 2019 versus 2022. Despite accounting for the same types of roles, the response population could be different each time.
Various healthcare professionals across the cancer care continuum were surveyed, including nurse practitioners, physicians, administrators, social workers/financial advocates (e.g., counselors and navigators), and other, which included pharmacists, nutritionists/dieticians, researchers, data managers, tumor registry staff, and more.
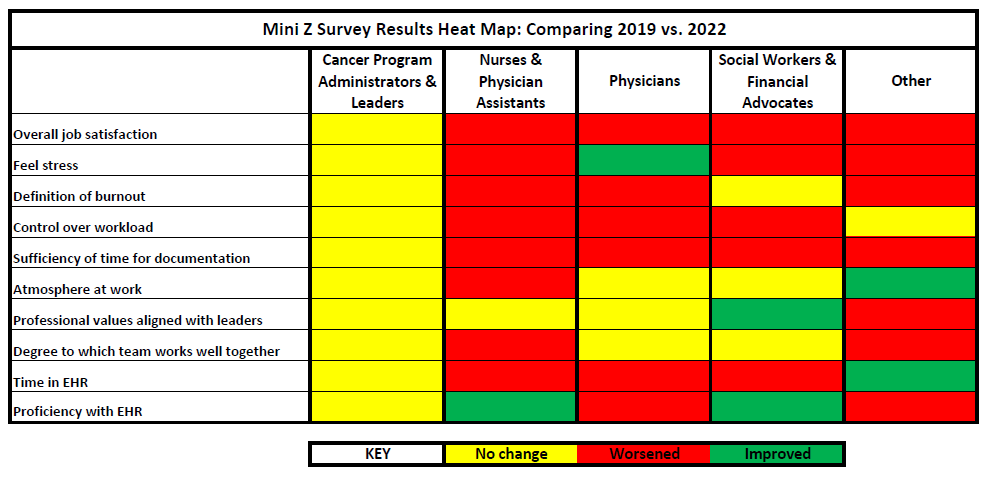
There was a lot of data to compare, and I tried to keep the analysis simple. To do so, I created a heat map to articulate the level of change or no change from 2019 to 2022. Yellow indicates that there was no change, red means there is increase in burnout, and green shows there was an improvement in burnout rates from 2019 to 2022 (see figure below).
Overall, among cancer program administrators and practice managers, there was no significant change in outcomes and indicators of burnout. If one were to speculate, you could argue that administrators love solving complex problems, and, perhaps, the pandemic had no effect on their overall perception of burnout. Further, the two most at-risk groups are—and have historically been—APPs and physicians.
Nurses and Physician Assistants
Results from the 2022 Mini Z show that for the outcome indicators of burnout (feeling stress, job satisfaction, defining burnout) nurses and physician assistants are worse now than in 2019. Survey results also show that the drivers of this increased burnout were a lack of control over work, insufficiency of time for documentation, negative workplace atmosphere, and teams not working well together. The one driver that did improve in this group was proficiency with the EHR.
Physicians
As previously noted, physicians have significant changes in their burnout outcomes and driver indicators compared to three years ago, although these changes are not as bad as what is observed in the nurse/physician assistant group. The physician data indicates that job satisfaction and feelings of burnout are, in fact, worse now than in 2019. However, the outcome indicator for burnout—feeling stressed—has improved within this group. Physicians also show no change in perception of their workplace atmosphere, alignment of their professional values with leadership, and the degree to which their teams work well together. Feelings toward time spent in the EHR, as well as EHR proficiency, are worse than 2019 survey results. This could likely be due to the complexities associated with EHR use and requirements for documentation, contributing to physician burnout.
Social Workers and Financial Advocates
For the social worker/financial advocate group, there is little change in the definition of burnout when compared to 2019 survey results. However, there is change related to job satisfaction and overall feelings of stress. Feelings about workloads and time for documentation are worsening, yet value alignment with leadership is improving. This group is the only one that shows a notable improvement in overall value alignment with leadership.
Other
The last category—including all the other healthcare professionals on the multidisciplinary cancer care team—saw job satisfaction, feelings of stress, and burnout rates worsen in 2022 when compared to 2019. Other drivers for burnout include the insufficiency of time for documentation and overall lack of proficiency with the EHR. Another interesting find: this group is the only one that saw a reduction in value alignment with leadership, meaning that this has worsened since the last survey in 2019.
What Can We Do to Combat Burnout?
As part of this survey, we also asked participants whether their cancer program or practice has taken any action or implemented any solutions to help mitigate staff burnout and promote resiliency. Among all survey participants, only about one-quarter answered in the affirmative. Another 18 percent were unsure if their program or practice had taken any steps to promote staff resiliency, and more than half responded that their program or practice had not. While all of our programs and practices likely understand the detrimental impact that burnout has on our care teams, it seems that relatively few of us know where to begin to tackle this complex problem.
I wrote about burnout and taking care of ourselves in one of my first blogs. It is so important that when we reflect on our team members who are at higher risk of burnout, we understand what is impacting their ability to find joy in the workplace and reduce job-related stress. Aside from the things that we have control over, being a strong advocate for and implementing recognition programs, good leadership, and time for clinical documentation and performing administrative tasks are just a few ways we can help our care teams improve on the key drivers of burnout measured in this survey.
Barbara Schmidtman, PhD, has worked in healthcare for more than 20 years in a variety of professional and clinical roles. Currently, she is the executive director of cancer health at Spectrum Health West Michigan in Grand Rapids. Dr. Schmidtman is the ACCC Workforce Subcommittee Chair, a subgroup of the association's Governmental Affairs Committee. Dr. Schmidtman earned her PhD in business administration from Northcentral University, where she specialized in industrial organizational psychology. Her doctoral studies focused on physician behaviors and how demonstrated physician leadership affects individuals and teams—either positively or negatively. Dr. Schmidtman has a passion for speaking locally and nationally on leadership styles and approaches.